In This Issue
Director's Message:
 VSI Hires New Staff Member: VSI Hires New Staff Member:
Meet Jean Pickford!
Support VSI
Which Treatment? Which Doctor?
What You Need to Know
Medicare Coverage for
Vitiligo Treatments
What's On Your Mind?
- Self-Tanning:
Tips and Techniques for Vitiligo
Medical News Updates
- Home Phototherapy for Vitiligo
- Zinc Deficiency and Vitiligo
Research & Clinical Trials
Bibliography and Sources
Shop Online: Earn Funding for
VSI with Amazon and eBay
 Now Visit VSI Now Visit VSI
on Facebook
 And Twitter And Twitter
View Past Newsletters
VSI Medical and Scientific
Advisory Committee
- Pearl E. Grimes, M.D., Committee Chair
- Ted A. Grossbart, Ph.D.
- Sancy A. Leachman, M.D.
- I. Caroline Le Poole Ph.D.
- Mauro Picardo, M.D.
- Nanette B. Silverberg, M.D.
- Richard A. Spritz, M.D.
- Alain Taieb, M.D., Ph.D.
- Wiete Westerhof, MD, Ph.D.
|
| |
| |
How to Log In:
Have you have forgotten your Login ID and/or Password?
No Problem!
Just go to the
Community Page
Scroll down to
the login box.
LOOK UNDERNEATH!
You'll see instructions to have them sent to the email address on your account. |
|
How to Log In:
Have you have forgotten your Login ID and/or Password?
No Problem!
Just go to the
Community Page
Scroll down to
the login box.
LOOK UNDERNEATH!
You'll see instructions to have them sent to the email address on your account.
|
|
How to Log In:
Have you have forgotten your Login ID and/or Password?
No Problem!
Just go to the
Community Page
Scroll down to
the login box.
LOOK UNDERNEATH!
You'll see instructions to have them sent to the email address on your account.
|
|
How to Log In:
Have you have forgotten your Login ID and/or Password?
No Problem!
Just go to the
Community Page
Scroll down to
the login box.
LOOK UNDERNEATH!
You'll see instructions to have them sent to the email address on your account.
|
|
| |
| Contact Us
Online
VitiligoSupport.org
Email Contact Us
Postal Mail Address
Vitiligo Support International
P.O. Box 3565
Lynchburg Va 24503
Phone
(434) 326-5380 |
|
|
Message From the Executive Director
 Dear VSI Members, Friends and Donors, Dear VSI Members, Friends and Donors,
The VSI Board of Directors and I have very exciting news to share with you!
On June 1, 2017, we welcomed Jean Pickford to the VSI staff as VSI’s Director of Development. Jean brings a wealth of knowledge and experience to the organization, and most importantly, she brings a passion for relationship-building, fundraising, organizational development, and member engagement. Read on to learn more about Jean!
Sincerely,

Message from Jean
 When Jackie asked me to write a brief introduction about myself for this newsletter, I had a lot of thoughts whirling around in my head. How can I express my excitement about being on the staff at VSI? How can my involvement directly impact VSI’s members who cope daily living with vitiligo? And, most importantly, how can I inspire the vitiligo community to give financially to help VSI move the needle towards an improved quality of life? When Jackie asked me to write a brief introduction about myself for this newsletter, I had a lot of thoughts whirling around in my head. How can I express my excitement about being on the staff at VSI? How can my involvement directly impact VSI’s members who cope daily living with vitiligo? And, most importantly, how can I inspire the vitiligo community to give financially to help VSI move the needle towards an improved quality of life?
I decided the best way to introduce myself to you was to write from my heart. And, hopefully you will be able to capture a little bit of my personality through these next few paragraphs. I have dedicated my working career to nonprofit patient advocacy helping individuals, families, and their caregivers.
I strongly believe that all patients should have access to reliable
and accurate information and contact with knowledgeable physicians.
When living with a chronic disease, patients should be empowered to be active participants in research and have the opportunity to engage with a community who understands and relates to the same issues and concerns.
The key to the overall success at VSI is developing and sustaining relationships with the stakeholders of the organization as well as providing an infrastructure to advance the mission. I’m honored that Jackie and the board have chosen me for this new role and I look forward to engaging with this amazing community.
Please look forward to more communications from me in the very near future.
In the meantime, if you have an idea to get more involved, or just want to chat, let me know!
Warm regards,
Jean
To send Jean an email: Click here
We’d like to take this opportunity to extend our most heartfelt gratitude
to each and every VSI Supporting Member and Donor.
As a nonprofit organization, all of VSI’s efforts: publications, programs, services, professional meetings and memberships, our office (staffed 5 days a week), server space, website, IT programmers, newsletter software, and much more, is sustained by the generous support of our donors.
If each person reading this newsletter made an annual donation
of just $10.00, VSI could nearly double its 2017 income.
Every Dollar Counts!
Will You Support VSI’s Campaign to Transform the Future of Vitiligo?
|
Back to Top

Which Treatment? Which Doctor?
What You Need to Know and How to Prepare
If you recently developed vitiligo, are seeing a doctor for the first time, or maybe a new or different doctor, you likely have a lot of questions. Whether you are one of the lucky ones who happens to have a vitiligo specialist in your area, or, if you are seeing a dermatologist who’s never treated a vitiligo patient, there are things you can do in advance of your appointment so that you and your doctor get the most from the time you have together.
One of the first, and most important steps you can take is to educate yourself about vitiligo and current treatments so that you’ll know what your options are and which treatment/s might work best for you and your lifestyle.
Treatment Background
Generalized vitiligo, the most common type, is an autoimmune disease characterized by patchy light colored areas of pigment loss on the skin, caused by the body’s immune system mistakenly attacking and killing the pigment-making cells, known as melanocytes.
Most vitiligo treatments fall into one of two categories:
Immunosuppressive: Treatments that suppress the melanocyte destruction
Immunoregulatory: Treatments that promote melanocyte repopulation
There are 3 primary types of treatment used for repigmentation.
Topicals - such as mid-to-potent strength topical corticosteroids like clobetasol, and calcineurin inhibitors like Protopic (tacrolimus), and Elidel (pimecrolimus)
These suppress the melanocyte destruction
Phototherapy - such as narrowband UVB (NB-UVB), UVA, and excimer laser
These promote melanocyte repopulation
Surgical - such as tissue and cellular grafts
These replace the areas of vitiligo with normal skin and/or cells
Treatments and Expectations
Topical treatments: (ointments and creams)
  Topical treatments alone usually take longer to produce results than either light alone or a topical combined with light. Depending on the area of the body, with a topical alone, results might not be evident for 8 months or longer. Topicals combined with light generally produce results more quickly than with light alone. Topical treatments alone usually take longer to produce results than either light alone or a topical combined with light. Depending on the area of the body, with a topical alone, results might not be evident for 8 months or longer. Topicals combined with light generally produce results more quickly than with light alone.
Mid - to super-high-potency topical steroids are suggested as the initial therapy for limited vitiligo (<10 percent of the total body surface area) and are used once daily for two to three months, followed by a one month rest.
Click here to view a topical steroid potency chart
 Topical calcineurin inhibitors (tacrolimus and pimecrolimus) are often preferred (rather than the potent topical steroids) for patients with limited disease involving the face or other areas at higher risk for skin atrophy. They are applied twice daily, or can be used in combination with a topical steroid, applying each medication once daily. Topical calcineurin inhibitors (tacrolimus and pimecrolimus) are often preferred (rather than the potent topical steroids) for patients with limited disease involving the face or other areas at higher risk for skin atrophy. They are applied twice daily, or can be used in combination with a topical steroid, applying each medication once daily.
Light Treatments:
  NB-UVB: Due to its safety profile, NB-UVB phototherapy is now the gold standard light treatment for vitiligo, and the initial treatment of choice for patients with vitiligo involving >10 percent of the body surface area (BSA). NB-UVB: Due to its safety profile, NB-UVB phototherapy is now the gold standard light treatment for vitiligo, and the initial treatment of choice for patients with vitiligo involving >10 percent of the body surface area (BSA).
Treating two to three times per week on non-consecutive days is considered optimal by most. Depending on the area of the body and degree of depigmentation, treatments can take from 6 months two years. Because research indicates no increased risk of cancer from NB-UVB, there are no recommendations for a maximum number of treatments.
This treatment may be used in a physician’s office, or, with a doctor’s prescription, home-light units may be purchased to use in the convenience of your home.
 Excimer Laser: Excimer uses a wavelength similar to NB-UVB,but delivers a targeted, narrow beam. It is very effective, but because of the size of the beam it is used to treat very small spots of depigmentation. Some doctors will begin with laser therapy for patients who have only a couple of very small areas of depigmentation. However, most doctors use laser for very small spots remaining after NB-UVB treatment. Excimer Laser: Excimer uses a wavelength similar to NB-UVB,but delivers a targeted, narrow beam. It is very effective, but because of the size of the beam it is used to treat very small spots of depigmentation. Some doctors will begin with laser therapy for patients who have only a couple of very small areas of depigmentation. However, most doctors use laser for very small spots remaining after NB-UVB treatment.
UVA/PUVA: Many years ago UVA light was combined with a chemical product, called a psoralen (which increased the body’s light sensitivity) for a treatment known as PUVA. Due to the many side effects, including skin cancer, this treatment has mostly been replaced by NB-UVB.
Surgical Procedures:
The best candidates for surgical therapies are those with stable segmental or localized vitiligo, or non-segmental vitiligo on stable areas that are difficult to treat, such as hands and feet, that have not responded well to mainstream treatments.
Segmental vitiligo starts and stays on one side of the body, spreads rapidly at onset then becomes stable, is most often seen in children aged 12 and under, and is not typically associated with autoimmunity.
Non-segmental vitiligo occurs on both sides of the body, often in a mirror type manner, and usually has an autoimmune disease component. |
Surgical therapies involve transplanting functional melanocytes (pigment cells) to de-pigmented areas, using methods such as tissue grafts, cellular grafts, or cellular transplantation.
Stability is generally defined as having no new lesions, no Koebner phenomenon (spreading as a result of skin trauma) and no spreading of current lesions in the previous 12 months.
Depigmentation Therapy:
For those with extensive pigment loss that has not responded well to above therapies, depigmentation of the remaining pigment is an option. This therapy uses a topical medication called monobenzyl ether of hydroquinone (monobenzone). This is a systemic treatment, meaning that it will cause depigmentation both locally (where applied) and remotely (on areas where not applied).
Monobenzone can be applied once or twice daily, beginning with the exposed areas. If a rash occurs in more sensitive areas, like the face, it can be continued on other less sensitive areas. Remote areas not receiving the medication will begin lightening after 3 to 6 months.
Therapy typically begins with monobenzone 10%. If that is well tolerated for the first month, the therapy can be increased to 20%. Depending on the individual, complete depigmentation may take from one to three years.
Side effects include contact dermatitis (rash), itching, and dry skin.
VSI has a very active Depigmentation forum where members discuss their depigmentation journey. This forum also provides information on pharmacies that can make and ship monobenzone.
Treatment Considerations:
Area and Amount of Involvement
The effectiveness and risk of a vitiligo therapy is directly related to the size of the treatment area(s). For example, a therapy that is very effective in repigmenting small areas of your skin may be much less effective treating large areas, and may also pose more risk. Topical steroids are a great example of this type of therapy.
Generally, the rule of thumb for the physician is that depigmentation involving 10% or less of the BSA is treated by a topical therapy. Combination therapy with a topical and light is usually considered when more than 10% of the skin is depigmented. Generalized depigmentation of more than 50% of skin may best be treated by depigmentation therapy.
Age of Patient
A patient’s age can affect selection of treatment. For example, though high-strength topical steroids have been reported to be effective in children, less potent steroids are often preferred in children under the age of 10 to minimize risk. A systemic steroid would not be used in a child.
Date of Disease Onset
Some therapies work best when used early/soon after disease onset. Topical steroids, for example, are considered to be most effective on small, newly de-pigmented areas, especially those on the face and neck.
Disease Activity
If the vitiligo is spreading quickly with widespread pigment loss, it may be necessary to use some type of systemic treatment to stabilize the vitiligo. Some physicians recommend low-dose oral corticosteroids such as prednisone, oral mini-pulse therapy with dexamethasone, or intramuscular triamcinolone; however, the response is better when used as an adjunct therapy to NB-UVB.
Emotional Component and Quality of Life
The emotional stress of vitiligo can have a very direct impact on the quality of life and should be taken into account. Even a small percentage of involvement can cause a great deal of emotional stress, particularly if more visible areas are affected. Under these circumstances, a doctor may consider a treatment prescribed more often for widespread vitiligo, such as a combination of a topical and light.
Location of Vitiligo
Generally, results of any treatment are better on the face and neck, followed by the trunk, upper arms, and upper legs. Feet and hands are among the most difficult to treat. Topical creams or ointments and light treatment are often prescribed for the more responsive areas. Surgical options can be considered for the less responsive areas.
Time Investment, Cost, and Insurance Coverage
 Vitiligo treatments can not only be expensive, but they also take time and commitment. When you start a treatment, you need to be prepared to continue consistent use as directed by your physician, long enough to obtain acceptable results. Depending on the circumstances, it may take 3-6 months to even begin seeing results, and 1 to 2 years for optimal results. Vitiligo treatments can not only be expensive, but they also take time and commitment. When you start a treatment, you need to be prepared to continue consistent use as directed by your physician, long enough to obtain acceptable results. Depending on the circumstances, it may take 3-6 months to even begin seeing results, and 1 to 2 years for optimal results.
Though the situation is vastly improved in recent years, some insurance companies will still try to use excuses for denial of coverage, such as the treatment being considered cosmetic, or experimental. If you have trouble obtaining insurance coverage, contact VSI and provide the reason the insurance company provided as reason for denial, and we can provide documentation to help. If you do not have insurance, you can ask your doctor for recommendations on receiving a reduced rate so that you can afford the treatment.
Lifestyle
Light treatments are typically prescribed to be used 2 or 3 days a week for several months or longer. It can be quite difficult to interrupt daily schedules (job, school, parents with young children, etc.) to go to a doctor’s office three days a week during office hours. After establishing a positive response from light treatment, you could discuss the possibility of your doctor writing a prescription for a home light unit.
Research has shown that those with home light units often have better outcomes because of the ease of use, as well as reduced long-term cost. With or without insurance, having a home light unit removes the cost of office visits and co-pays.
Underlying Conditions:
If a person has lost quite a bit of pigment in a very short time, it may be necessary to determine and treat the cause. Some underlying conditions frequently seen with vitiligo are autoimmune thyroid disease, type 1 diabetes, rheumatoid arthritis, celiac disease, and vitamin D deficiency.
Background Information for Your Physician

Disease History
- When did you first notice pigment loss?
- Were there precipitating factors, such as sunburn or illness?
- Did the vitiligo begin slowly and spread slowly?
- Did you notice many small areas over the entire body?
- Did it begin rapidly and spread quickly?
Family History: Have you or anyone in your family experienced any of the following:
- Early graying/white hair
- Alopecia areata
- Thyroid disease (either hypo - or hyperthyroid)
- Psoriasis
- Insulin-dependent diabetes
- Pernicious anemia
- Addison's disease
- Celiac disease
Treatment History/Experience: If you previously used a vitiligo treatment.......
- How long ago did you see the prescribing doctor?
- Are you currently using any medications?
- Are you currently using any type of vitiligo treatment? If so, what?
- Which vitiligo treatment/s have you ever used?
- How did you use the treatment? For example, if it was a topical treatment, how many times a day did you apply it? How long did you leave it on? How many days a week did you apply it?
- How long did you use the treatment? (days, weeks, months)
- Describe any results.
- Did you experience side effects? If so, what were they?
Diagnosis and Evaluation Procedures:
Each doctor's protocol will differ but the following are the more common procedures:
- a total body skin examination
- observation with a Wood's lamp (similar to a black light)
- photographs, in order to track progress on follow-up exams
Many doctors will order laboratory tests to assist his/her evaluation of the vitiligo.
Some of the more typical tests include all or part of the following:
Antinuclear Antibody (ANA) - helps determine if the patient has other autoimmune diseases.
Complete Blood Count (CBC) with differential
Comprehensive Metabolic Panel: Research has shown an increased risk of those with vitiligo
developing metabolic syndrome.
Thyroid panel tests listed below: The risk for those with vitiligo of developing autoimmune thyroid disease (AITD) has been found to be 2.5 times higher than in the normal population.
- Free T3: Measures blood level of T3 hormone that is unbound, meaning that it is available to be used by cells and tissues.
OR
T3 (Total T3): When not preceded by the word “Free,” it is referring to the “Total” amount, which includes both bound (unavailable) and unbound (available) hormones.
- Free T4: Measures blood level of T4 hormone that is unbound, meaning that it is available to be used by cells and tissues.
- TPO test: Commonly used to detect autoimmune thyroid disease by identifying antibodies directed against thyroid peroxidase (TPO).
- TSH test: Measures the level of thyroid stimulating hormone (TSH) in the blood, ordered when signs or symptoms of an overactive or underactive thyroid condition is suspected or diagnosed, or to monitor for those conditions.
25-Hydroxy-Vitamin D - also known as 25(OH)D:Vitamin D is an area of deficiency for many vitiligo patients.
Folate/B12: Research has found that many vitiligo patients are also deficient in B12 and folate.
Treatment Questions:
If your doctor recommends a treatment, knowing the information below may help with your decisions:
- How does this treatment work to help vitiligo?
- What are its possible side effects?
- How is it used and how often?
- If topical, can it be washed off? If so, after how long?
- If you want to apply sunscreen and the topical medication, which would you apply first?
- What type of results might you expect to see?
- How long will it take for me to see results?
- How long will you use this treatment?
- Does insurance normally cover the treatment? If not, can the doctor help to secure coverage?
- How much will the treatment cost?
Having a friend or family member come along, and/or taking a tape recorder on
your office visit, may be useful in recalling instructions or information later. |
Finding a Doctor
Now that you’ve done your homework and are ready to make an appointment, if you don’t have a vitiligo specialist nearby, what can you do?
Although any doctor can write a prescription for a vitiligo treatment, typically skin conditions like vitiligo are seen by a dermatologist. However, in many smaller cities it can be quite difficult to find a dermatologist who is taking new patients, and those that do, can have waiting times of 6 months or longer for an appointment.
If this happens, be sure to ask if they have a “cancellation list” to which your name can be added. If they do not, then ask the best time to call each day to check for cancellations.
Another problem frequently encountered is that a great number of dermatologists have outdated beliefs and/or information on the safety and efficacy of current vitiligo treatments, and will not prescribe them.
VSI has a “Doctor Search” which, after logging on to your account, can be accessed from the Community tab. The doctors on this list have been seen by VSI members who liked them and submitted their information. If you locate a doctor listed near you, open their page to see if the treatment you are seeking is listed. You should always double check when you call the office to be sure the information is still accurate.
If you do not see a doctor listed near you, this does not mean there aren’t any vitiligo knowledgeable doctors in your area, just that none have been submitted to VSI. Your next step would be to use a computer search with words like vitiligo dermatologist, and your city. If that also is unsuccessful, just begin calling dermatology offices and ask if any of the doctors have treated vitiligo patients, and if so, which treatments they prescribe.
If you still haven’t found a dermatologist who has treated other vitiligo patients, you can contact VSI for peer-reviewed information on vitiligo treatments to print and take with you.

Back to Top
Calling all Medicare Vitiligo Patients!
  VSI regularly hears from patients from all over the United States who have been denied insurance coverage for their vitiligo treatment. VSI has been fighting this battle on a national level for several years. While we are definitely making progress, it’s been a slow road. VSI regularly hears from patients from all over the United States who have been denied insurance coverage for their vitiligo treatment. VSI has been fighting this battle on a national level for several years. While we are definitely making progress, it’s been a slow road.
Part of the problem is that currently there is no accepted standard for coverage of vitiligo treatments. Each company has their own policies and guidelines, many times based on outdated and incorrect information.
What most people may not realize is just how much private insurance coverage can be affected by Medicare policies. Over 55 million Americans are now covered by Medicare or Medicare Advantage, making it the nation’s largest health insurance program. Consequently, many, if not most, insurance providers establish their baseline standards and procedures to follow the Medicare model.
We have been in touch with Medicare and have been told that if we can provide a Medicare letter of denial for a vitiligo treatment, then they will try to help us set a standard of coverage.
If you are reading this newsletter and you, or someone you know, was denied coverage for a vitiligo treatment by Medicare, please contact VSI immediately. You could help make a difference for future insurance coverage for ALL vitiligo patients! Click Here to Contact VSI


What's On Your Mind?
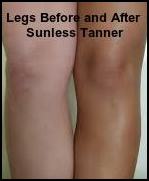
Q. I have vitiligo on my hands, arms, and legs and in the summer the contrast makes the vitiligo even more noticeable. I really need something to help even out the color. I tried some self-tanners but they turned the vitiligo an orangey color which looked very unnatural compared to the rest of my skin. Can you recommend a product or technique I could use to help make these areas less noticeable?
Dihydroxyacetone (DHA) and Sunless Tanners
- Many people shy away from sunless tanning products because of the reputation they had in the early days for producing a very unnatural orange color. Though some may still do so, many advances in recent years have not only reduced the orange, but have added multiple shades and colors. However, application technique is very important.
 DHA-based sunless tanners come in many different formulations, such as lotions, gels, liquids, sprays, mousses, wipes, and even airbrush applications, most of which can be purchased in drug stores, big box stores, and online. Some products offer both an immediate tint as well as DHA that will take longer to develop color. Spray tanning products and businesses have also become very popular, offering a wide range of choices from home airbrush systems to full body spray booths. DHA-based sunless tanners come in many different formulations, such as lotions, gels, liquids, sprays, mousses, wipes, and even airbrush applications, most of which can be purchased in drug stores, big box stores, and online. Some products offer both an immediate tint as well as DHA that will take longer to develop color. Spray tanning products and businesses have also become very popular, offering a wide range of choices from home airbrush systems to full body spray booths.
DHA products are no longer “one-color-fits-all.” The DHA concentration of commercial products can range from 2.5 to 10% or more, but most fall within the 3-5% range. The higher the percentage of DHA, the darker the color it will produce. Some of the labels make it difficult to know exactly how light or dark the product will actually look on your skin, but terms such as “fair” or “light to medium” generally produce a lighter color and terms like “deep” or “dark” are darker.
Most of the sunless tanning products are not marketed as corrective products for skin conditions, but there are application “tips and tricks” that with a little practice can be used to more successfully cover vitiligo.
Self-Tanner Tips:
Always begin by carefully reading the label! This will help you learn if the product is a lighter or darker shade, if it has any immediate color or tint, how quickly the DHA color will develop, how long the color will last, if it produces a shimmery look that will make your skin glisten, and precautions such as not inhaling or the need to cover fingernails.
Blending: The art of blending will be an ongoing process. If you are using a spray to cover a larger area, do not worry too much about precision. You’ll want to apply extra to the depigmented area, but you want that area to eventually blend into the pigmented area, so overlap is ok. The same is true of the gels and lotions. After applying the product to the depigmented area, try to “feather it” outward so as not to leave a stark line of demarcation.
Camouflage: As mentioned above, reducing the contrast between the pigmented and depigmented areas is the key to successful blending and camouflage. This can be achieved in various ways, but with the sunless tanners, you begin by applying an extra or heavier coat over the lighter area, then applying another coat over the entire area.
Drying: Different products suggest different drying times. Many people use a hair dryer after applying to help set the product. If using a spray tanner, you might want to use a lower power setting on the dryer so you do not risk creating ripples or streaks from blowing the wet spray. Lotions and gels seem to stay a bit tacky even after the recommended drying time. If using a lotion or gel at night you might want to apply a couple of hours before bedtime to be certain it is well set.
Be patient: Allow adequate time for DHA to develop before applying another coat, especially on obvious places like the face or hands.
Patch Test: If you are using a product for the first time, it might be a good idea to use it on a small, sensitive area, such as the inside of your arm or on your stomach, then wait 24 hours to be sure you are not allergic to any of the ingredients.
What Type of Product to Use: If the depigmented area is greater than a few inches, you might try a product with broader coverage capability such as a spray, gel, or lotion. However, if the depigmented area is smaller, and particularly if it is in a very obvious location (like the face or hands), you may benefit from a product capable of a more precise application, such as Chromelin Complexion Blender. This is a concentrated liquid DHA product, and one of very few specifically developed for skin conditions like vitiligo. It is applied with a small applicator directly to the affected area. After applying the Chromelin, you can then coat the entire area with a DHA spray or lotion. It may take some trial and error to accomplish blending the two areas; just keep in mind that the DHA in different products may produce different shades and develop at different rates.
Self-Tanner Terms:
Bronzer: Bronzers typically are makeup-type products that produce instant, but temporary, color that can be washed off at the end of the day. Some examples are tinted moisturizers and brush-on powders, and they  may use the terms “instant tan” or “tint” in addition to “bronzer.” Sometimes these products are combined in the same product with DHA, (check the label) giving you a level of instant coverage to provide extra camouflage, in addition to the color that develops over time and lasts several days. This can be particularly helpful for covering vitiligo. You can apply the tinted formula to the depigmented area either alone, if it matches the surrounding skin, or as a base using a heavier or repeated application to the lighter skin, then cover the entire area afterwards to blend together. may use the terms “instant tan” or “tint” in addition to “bronzer.” Sometimes these products are combined in the same product with DHA, (check the label) giving you a level of instant coverage to provide extra camouflage, in addition to the color that develops over time and lasts several days. This can be particularly helpful for covering vitiligo. You can apply the tinted formula to the depigmented area either alone, if it matches the surrounding skin, or as a base using a heavier or repeated application to the lighter skin, then cover the entire area afterwards to blend together.
Another benefit of the combination products is that the instant color allows you to see exactly where you are applying, and may help reduce missed areas, streaks and over-application. Always check labels and ingredients to see exactly what the product you are using contains.
Exfoliate: The DHA chemical works on the top layer, which is dead skin. Areas of thicker, rougher skin such as the knees, hands, elbows, and ankles may absorb more of the tanning solution, resulting in a darker, uneven color. For best results, exfoliation is recommended prior to applying self-tanner to evenly remove as much of the dead skin as possible.
Self-Tanning Moisturizer: These have a lower concentration of DHA and provide just a hint of color.
Shimmer: Labels that use words like “shimmer” or “iridescent” generally mean the product leaves a glittery appearance on the skin. This may work better for some than others. It may be more difficult to convince others that your color is natural if you’re shimmering like a fairy.
Commercial Product Examples
Self-Tanning Moisturizer: Jergens Natural Glow Daily Moisturizer
Sunless Tanning Spray: L’Oreal Sublime Bronze Self-Tanning Mist
(does not contain a bronzer)
Tinted Self-Tanning Lotion: L’Oreal Sublime Bronze Tinted Self-Tanning Lotion (label mentions “Instant Shimmer” which means it will have a glittery appearance)
Gel: Sublime Bronze Self-Tanning Gelee
(does not contain a bronzer – does not mention shimmer)
Combination DHA and Bronzer:
St. Tropez Self Tan Bronzing Mousse – Available in Light and Dark Bronzing
PretendTan – Darker Bronzer
St. Moriz Instant Self-Tanning Mousse -- Available in multiple shades
Liquid DHA with Applicator:
Chromelin Complexion Blender |
The above information is an excerpt from VSI’s Summer
2015 Newsletter article “Corrective Cosmetics: Tips for Vitiligo.”
For additional information, or to view in its entirety: Click Here.

Medical News Updates
Highlights of recently-published medical
articles on vitiligo and its treatments
Home Phototherapy for Vitiligo
Researchers and clinicians from Henry Ford Hospital in Detroit, MI and from Medicine Siriraj Hospital in Bangkok, Thailand published an article about the safety and efficacy of home phototherapy using narrowband UVB (NB-UVB) in an effort to dispel misconceptions and increase awareness and use of this vitiligo treatment.
 
The authors noted that psoralen plus ultraviolet A (PUVA) was the standard vitiligo treatment for many years, but due to its many drawbacks, such as nausea, vomiting, phototoxicity, and skin cancer, NB-UVB has now become the standard of care for vitiligo.
When compared to PUVA, NB-UVB is as effective (with far fewer adverse side effects), produces a better repigmentation color match, and has a faster rate of repigmentation. However, due to the long-term time commitment and associated costs, its use in physicians’ offices has been somewhat limited. An alternative, home phototherapy, is a far more convenient and cost effective option, but often underutilized due to a lack of physician training and experience, as well misconceptions regarding safety and efficacy.
Safety
Physicians cited safety concerns as a primary barrier to prescribing home phototherapy. However, multiple studies have shown that when patients are properly educated on its proper use, adverse side effects are quite low and similar to those experienced in-office, such as the skin getting too red, burning, dryness, and itching.
Home therapeutic devices can be equipped with safety measures to prevent over-use side effects. These features include controlled prescription timers, that allow a fixed a number of treatments, after which a new code from the patient’s physician is required; timers limiting the length of treatment; and electronic data loggers enabling physicians to track patient usage and adherence.
The authors also pointed out that the patients at highest risk for side effects from a home light unit are those who purchase light units independently and self-administer without medical oversight.
Efficacy
A perceived lack of efficacy was found to be another significant barrier to physicians prescribing home phototherapy. “55% of 367 surveyed dermatologists believed that in-office phototherapy was superior to home phototherapy.” However, previous studies indicate that home phototherapy is equally effective as in-office therapy and decreases the patient burden, resulting in greater compliance.
Patients who are good candidates for in-office phototherapy should be considered for home phototherapy. Requirements include motivation, ability to comply with instructions, and willingness to return to the clinic periodically for reevaluation.
The authors concluded that based on current literature, home phototherapy is safe and effective and eases many of the hardships associated with in-office phototherapy, and should therefore be considered in the management of vitiligo. They cited “a knowledge gap on home phototherapy among many providers,” and recommended that further education be provided.
Zinc Deficiency and Vitiligo
Over the years, a variety of research studies have noted an association between serum zinc levels and vitiligo, yet you do not often hear much about this connection. In April 2017, a group of Iranian researchers reported the results of a prospective cross-sectional study comparing serum zinc levels of 100 vitiligo patients to those of 100 healthy (non-vitiligo) controls.
They noted that apoptosis (cell death) of melanocytes (pigment-making cells) is a primary cause of pigment loss in vitiligo. Because zinc is known for its anti-apoptotic properties, as well as being one of several micronutrients playing an important role in the process of melanogenesis (the production of melanin), they proposed the potential of zinc helping to prevent and/or control vitiligo.
The results of their study showed significantly lower serum zinc levels in the vitiligo patients compared to the control group, which they felt highlighted the role of zinc in the development of vitiligo. They suggested conducting large-scale studies to confirm their findings and to determine the outcome of oral zinc supplements for vitiligo patients.
-------------------------
Additional Zinc Facts
Zinc and copper have a very close relationship and work best in the range of 8:1 to 12:1 zinc to copper ratio. When properly balanced, they work synergistically. However, the intake of one has a direct and inverse relationship on the other. In addition to exposure or consumption, factors such as stress or diet can reduce zinc levels, causing an increase in copper, and over time create an unhealthy imbalance.

Back to Top
Research & Clinical Trials
Online Vitiligo "Selfie" Study!
Vitiligo Selfie Study
Research Coordinator: Elizabeth Tkachenko

Online Study Conducted by:
University of Massachusetts Medical School
Department of Dermatology
The goal of this study is to observe how vitiligo changes, moves, or resolves over time using self-taken, “selfie” photographs.
If you choose to participate, you will send us one photo per week for 52 weeks (one year). By combining and tracking these photos, we will be able to determine how the lesions in vitiligo tend to change and progress over time.
The entire study will take place online, and you will receive weekly email reminders containing a direct link to the short survey and secure photo-upload feature.
We are looking for participants with darker skin tones who are currently not receiving any treatment for their vitiligo.
If you are interested in participating, please contact research staff and we can send more information, answer your questions, and determine if you are eligible to participate in the study. Contact: [email protected] |
Vitiligo Research Study in New York City.
Volunteers Wanted
Have you been diagnosed with vitiligo?
Would you like to take part in a research study
to help those who have been diagnosed?
We are looking for both healthy volunteers and persons diagnosed with vitiligo to take part in a research study.
We are recruiting from the NYC areas since volunteers must visit our clinic on two separate occasions.
The biology of vitiligo is poorly understood and while there are many treatment options, many carry the risk of side effects or are only temporarily effective. We are performing a study to improve our understanding of the biology of vitiligo. Subjects will be asked to come to 2 study visits. We will be collecting skin samples from both patients diagnosed with vitiligo as well as healthy adults for this study.
We will compare pigment cells from the two groups to identify differences that may contribute to progression of vitiligo. This is not a treatment trial. This information may allow us to develop improved treatments for vitiligo.
Study visits will take place at:
The Dermatology Clinical Studies Unit
NYULMC Ambulatory Care Center
240 East 38th Street, 11th Floor
New York, NY 10016
For more information, please contact:
212-263-5244
[email protected]
IRB Approved For Period 10/4/16 – 10/3/17 |

Earn Funding for VSI with Amazon and eBay
Online Shopping Can Benefit VSI!
AMAZON SHOPPING
With thousands of items in addition to books, Amazon.com is a one stop-shopping center! Simply shop through the above link (bookmark it for easy reference) and VSI will earn fees, based on a percentage of the sale. The more items purchased by members, the higher the percentage! Our Vitiligo Library and Store, containing books, articles and products for those with vitiligo, is also powered by Amazon.
Tobi Cares Donation Program
Tobi is an online women's clothing design label that brings LA style from its design studio
direct to its online clothing store at tobi.com. Go to Tobi Cares and sign up for VSI to receive 1% of your purchase amount.
iGIVE SHOPPING
iGive.com offers access to free shipping deals and exclusive coupons, on top of the great deals you'll find every day through its network of 1,000+ stores, including Pottery Barn, REI, Staples, Petco, Expedia, Best Buy, QVC and many more. Best of all, up to 26% of your purchase at each store is donated to VSI at no cost to you! Let friends and family know so they can support VSI, too. Click register for iGive to get started today, and download the iGive button to automatically benefit VSI whenever you go to an included store. You can also raise a penny per search through iGive’s search engine, isearchigive.com.
GOODSEARCH SHOPPING AND DINING!
GoodSearch and Goodshop, like iGive, offers coupons, discounts, and donations to VSI through its network of over 5,000 stores. Just click the link above to get the savings started and the donations flowing!
* Vitiligo Support International Inc. (VSI) is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. |
Support VSI Through Ebay
Support VSI with eBay!
Do you sell items on eBay, or want to hold an online garage sale? If so, consider donating a percentage of your proceeds to VSI through eBay’s Giving Works program! It’s easy – when you list an item through a Giving Works listing, choose to send 10-100% of the final sale price to VSI. Your listing will have a special placement and designation. You’ll receive a proportional fee credit from eBay, and will also receive a tax donation receipt when the donation is deducted from your funds received. It’s a great opportunity to make some money for yourself and for VSI, so clean out those closets and garages and get selling!
To Learn More About VSI's Giving Works: Click here |
|




 When Jackie asked me to write a brief introduction about myself for this newsletter, I had a lot of thoughts whirling around in my head. How can I express my excitement about being on the staff at VSI? How can my involvement directly impact VSI’s members who cope daily living with vitiligo? And, most importantly, how can I inspire the vitiligo community to give financially to help VSI move the needle towards an improved quality of life?
When Jackie asked me to write a brief introduction about myself for this newsletter, I had a lot of thoughts whirling around in my head. How can I express my excitement about being on the staff at VSI? How can my involvement directly impact VSI’s members who cope daily living with vitiligo? And, most importantly, how can I inspire the vitiligo community to give financially to help VSI move the needle towards an improved quality of life? 

 Excimer Laser: Excimer uses a wavelength similar to NB-UVB,but delivers a targeted, narrow beam. It is very effective, but because of the size of the beam it is used to treat very small spots of depigmentation. Some doctors will begin with laser therapy for patients who have only a couple of very small areas of depigmentation. However, most doctors use laser for very small spots remaining after NB-UVB treatment.
Excimer Laser: Excimer uses a wavelength similar to NB-UVB,but delivers a targeted, narrow beam. It is very effective, but because of the size of the beam it is used to treat very small spots of depigmentation. Some doctors will begin with laser therapy for patients who have only a couple of very small areas of depigmentation. However, most doctors use laser for very small spots remaining after NB-UVB treatment. Vitiligo treatments can not only be expensive, but they also take time and commitment. When you start a treatment, you need to be prepared to continue consistent use as directed by your physician, long enough to obtain acceptable results. Depending on the circumstances, it may take 3-6 months to even begin seeing results, and 1 to 2 years for optimal results.
Vitiligo treatments can not only be expensive, but they also take time and commitment. When you start a treatment, you need to be prepared to continue consistent use as directed by your physician, long enough to obtain acceptable results. Depending on the circumstances, it may take 3-6 months to even begin seeing results, and 1 to 2 years for optimal results.



 DHA-based sunless tanners come in many different formulations, such as lotions, gels, liquids, sprays, mousses, wipes, and even airbrush applications, most of which can be purchased in drug stores, big box stores, and online. Some products offer both an immediate tint as well as DHA that will take longer to develop color. Spray tanning products and businesses have also become very popular, offering a wide range of choices from home airbrush systems to full body spray booths.
DHA-based sunless tanners come in many different formulations, such as lotions, gels, liquids, sprays, mousses, wipes, and even airbrush applications, most of which can be purchased in drug stores, big box stores, and online. Some products offer both an immediate tint as well as DHA that will take longer to develop color. Spray tanning products and businesses have also become very popular, offering a wide range of choices from home airbrush systems to full body spray booths.

